On Oct. 13, 2021, at 7:27 pm, beautiful Grace Schara—an inquisitive young woman with Down-Syndrome—died a tragic and preventable death at a Wisconsin hospital. Rather than using treatments proven to combat COVID-19, Ascension's St. Elizabeth's Hospital followed the U.S. government's ineffective COVID-19 treatment protocols, for which they reap significant financial rewards. On the final day of Grace's life, as her doctor assured her parents she was doing well, Dr. Gavin Shokar also "unilaterally labeled Grace a DNR and ordered a lethal combination of IV sedatives and narcotics"—a fatal combination of the drugs Precedex, Lorazepam, and Morphine—which were administered over an incredibly short period of time. Notably, all three drugs are manufactured by mRNA "vaccine" maker and pharmaceutical giant Pfizer.
Who Was Grace Schara?
Grace Schara was full of love. Properly describing the magical impact Grace had on every life she touched—especially her mom, dad, and sister—would require more space than this article. Her family and all those who knew and loved Grace were clearly blessed to have her in their lives for 19 years. Besides bringing an incredible amount of joy everywhere she went, Grace could read and write, drive a car, ride a horse, play the violin, and drive her riding lawnmower, and so much more. Truly, Grace loved absolutely everything about the life she was living. UncoverDC spoke at length with Scott Schara, Grace's father, about the tragic and immoral circumstances leading up to his daughter's death. Describing Grace, Scott recently wrote:
"Grace was our bright, beautiful, fun-loving 19-year-old daughter with Down Syndrome. Her precious life was taken from us at St. Elizabeth's Hospital in Appleton, Wisconsin, on Oct. 13, 2021. She was an angel who loved her Lord and Savior, Jesus. Everyone knew Grace. I was known only as 'Grace's dad.' She had a sense of her Heavenly Father that very few people ever have. She called me her 'Earthly dad.' Who does that?"
 Screenshot / Our Amazing Grace / Grace's Dad Remembers
Screenshot / Our Amazing Grace / Grace's Dad Remembers
[gallery size="full" ids="36742,36743,36744"]
What Happened? Hospital Neglect Leading to Grace's Last Day
On Sept. 28, Grace began receiving appropriate doses of Ivermectin when facing COVID-19 symptoms. On Oct. 1, with symptoms persisting, Grace's parents gave her a home COVID test. She tested positive, but they were prepared. Already following recommendations from America's Frontline Doctors and FLCCC, the Schara's had on hand the necessary essentials to work through COVID. Still, according to Scott, a few days later, "[Grace] couldn't maintain her oxygen above 90, so we ended up taking her to urgent care, which led to the emergency room. And the emergency room physician recommended that we admit her to the hospital."
The Emergency Department at Ascension's St. Elizabeth Hospital wanted to admit Grace. However, the hospital informed Scott that due to "hospital protocol not allowing anyone in the room," he could not come with her. Scott told the hospital that he would take Grace home if he could not go to the room with her. After "a meeting of the minds," he was told he could stay with his daughter as long as he didn't leave the room. Scott was fine with that, as he was not planning to leave the room anyway. So, Grace was admitted to the hospital. Further explaining how important it was he stay with Grace, Scott added:
"One of the things Grace was unable to do in this situation is to speak up or stand up for herself in terms of treatment and things like that. That's a natural part of what she was dealing with. And so, I did what any dad should do. I stood by my daughter and tried to protect her."
Grace's first full day in St. Elizabeth's was Oct. 7. Scott described the day as "very normal"—they watched movies and "horsed around." Scott explained that later in the day, Grace was frustrated and fighting back a little with the "high-flow cannula [that was] shooting air up her nostrils at 40 miles an hour or so." Clearly, Grace did not like the uncomfortable aspect of that treatment. On the morning of the second day, Oct. 8, Scott had the first real sense of "there's something going on here" when a doctor came into the room and told him:
"In the next two hours, we're going to have to put your daughter on a ventilator."
Immediately, Scott wanted to know the reasoning behind such a drastic decision. The directive turned out to be based on blood gas numbers from the previous night when Grace was aggravated with the cannula and "wrestling with a BiPAP mask." The situation had caused a blood pressure reading of 235/135 and a heart rate of 150 beats per minute. Knowing her elevated numbers were provoked by the situation the night before, Scott asked the hospital to retake them. They did, and just as he predicted, Grace was fine. Scott added:
"So we dodged the first ventilator bullet at that point."
The next day, Saturday, Oct. 9, Scott said Grace felt back to normal. She was hungry after not eating much the day before, and they ordered food off the menu. Once it arrived, Scott began feeding Grace. Swiftly, a nurse entered the room and told him that he could not feed Grace due to her 85% oxygen saturation. Not buying the 85% number, Scott (who had much of his COVID protocol with him after being told by the hospital that "he would get COVID-19 while there") retested Grace with his own oxygen saturation meter -it read 95%. He asked the nurse if his meter reading was correct, and she said it was. Thoroughly discouraged, Scott explained:
"The hospital's meter read 85%, so I put mine on, and it read 95%. I called the nurse back in, and I said, "is my oxygen meter accurate?" She said, "yes." I said, "well, why does yours only read 85% and mine reads 95%?"
[The nurse] admitted my meter was accurate and said hers was inaccurate. I asked why, and she said, "well, the leads get sweaty." I said, "if you know that, why don't you proactively change them out every four hours or whatever it needs to be?" She [sarcastically] said to me, "you should be thankful you caught this."
So process this reality. The primary statistic they're using to manage my daughter's care, including recommendations for all kinds of crazy things, including a ventilator, is the oxygen sat[uration]. Their oxygen saturation numbers are wrong, and they're recommending a ventilator based on that.
 Screenshot / Our Amazing Grace / Allocation of Care - Big Picture Agenda
Screenshot / Our Amazing Grace / Allocation of Care - Big Picture Agenda
Following the oxygen saturation fiasco, at 7 am on Sunday, Oct. 10, Scott explained that the head nurse came into Grace's room with an armed guard and told him he needed to leave. It is crucial to note that previously, Scott had been trained by the nurses on how to turn off the alarms in Grace's room so they didn't keep her up all night. Confused about the directive to leave the room, Scott asked what prompted this out-of-the-blue action. The nurse replied, "you've been shutting off the alarms at night." Scott explained to the head nurse that he was given the OK to turn off the alarms by other nurses at the hospital. She replied, "the main thing is the last three shifts of nurses don't want you in the room." With that, the armed guard escorted Scott to his truck. He shared:
"These alarms are going off twenty, thirty times a night, and oftentimes it's 30 minutes before the nurses come in. Of course, they don't want me in the room challenging these things. And so I got walked out by an armed guard. He walked me all the way out to my truck. We got to my truck, he said he listened to this back and forth for an hour. He said, "you've got to take this to a higher level." He knew what the deal was. Fortunately, our special needs attorney was available on Sunday, and I got a hold of her. She coached me on how to get my daughter Jessica in the room as a replacement advocate [Cindy could not be the advocate due to having COVID]."
Ready to go with her bags packed, on Monday, Oct. 11, Jessica was in Grace's room fifteen minutes after she was approved to go there. However, due to a lack of communication with the floor staff, Jessica could not stay overnight the first night and had to leave at 7 pm when visiting hours ended. She was with her sister all day on Tuesday, Oct. 12, watching movies and enjoying each other's company. Before Grace went to sleep, she had a FaceTime call with Jessica's boys—her two nephews—hollering, "hi boys!" The following morning, Wednesday, Oct. 13, the doctors called Scott and his wife and told them "how good of a day Grace had the day before."
 Our Amazing Grace / Thou Shall Not Kill
Our Amazing Grace / Thou Shall Not Kill
Grace's Last Day: The Alarmingly Cruel Facts
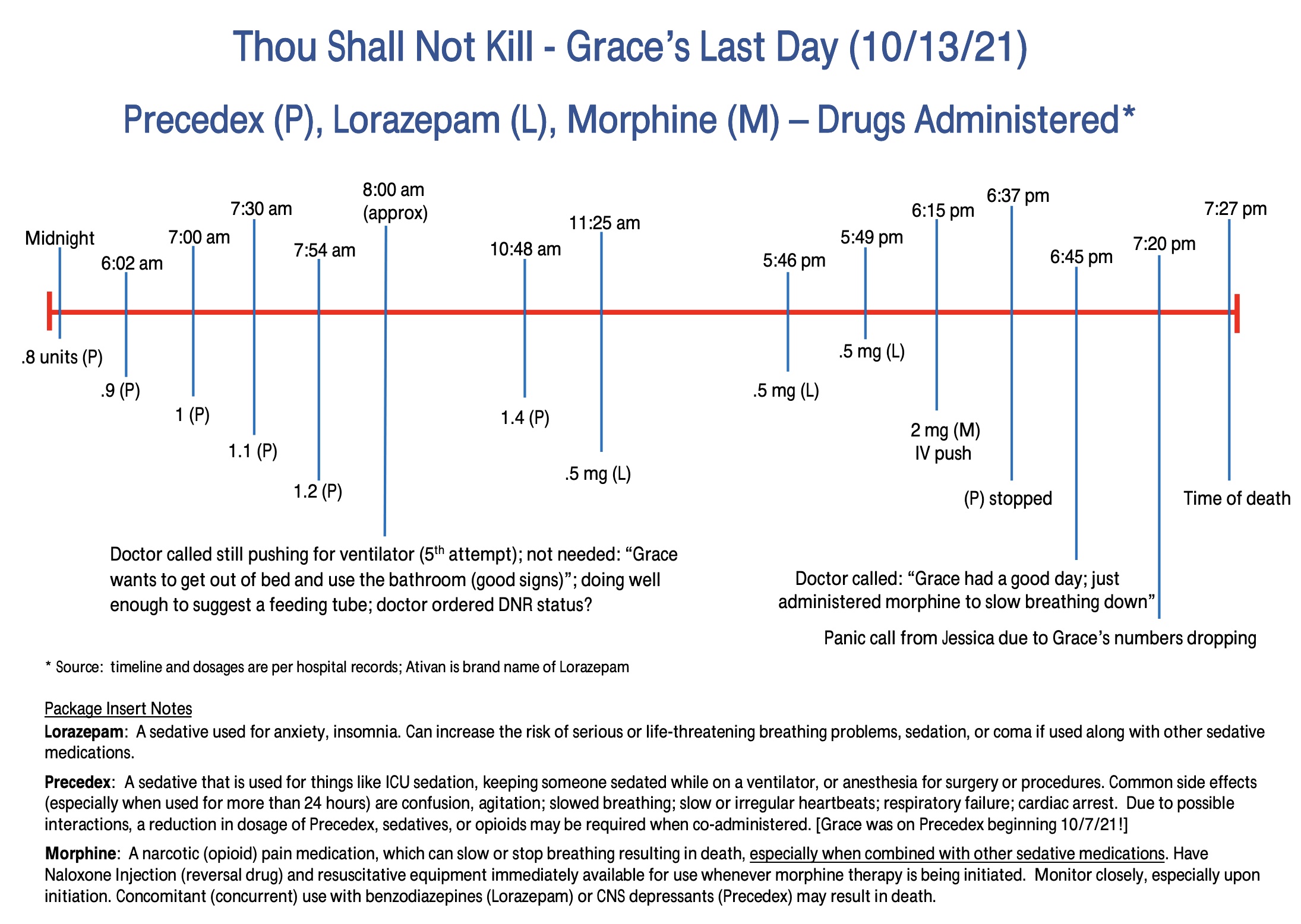
In the four days leading up to her death, Grace was given the Pfizer drug Precedex, a short-term sedative (to be used for 24 hours or less, according to the package insert). On Oct. 13, the day of Grace's death, nurse Hollee McInnis—under orders from Dr. Gavin Shokar—started "ratcheting up" the administration of Precedex. By 10:48 am, Grace (who was placed in restraints around 9 am that day for wanting to go to the bathroom) was receiving 14 times the initial dose.
Then, at 11:25 am on the day of her death, the hospital gave Grace a dose of the Pfizer drug Lorazepam. Next, at 5:46 and 5:49 pm—three minutes apart—they gave her two more doses of Lorazepam. Following that, at 6:15 pm, they gave Grace a two-milligram dose of Morphine—also manufactured by Pfizer—as an IV push, not a drip.
As shown below, in a bold warning, Pfizer's prescribing information for Morphine highlights the severe and life-threatening risk of "profound sedation, respiratory distress, coma, and death" when combined with benzodiazepines (in this case, Lorazepam) and CNS (central nervous system) depressants (in this case, Precedex). Additionally, the insert clearly states, "Have Naloxone Injection and resuscitative equipment immediately available." As emphasized by a heartbroken Scott, the hospital did not have the reversal drug Naloxone at Grace's bedside ready to go if needed.
 Our Amazing Grace / Morphine Package Insert
Our Amazing Grace / Morphine Package Insert
 Screenshot / Our Amazing Grace / Precedex notes from doctor and nurse
Screenshot / Our Amazing Grace / Precedex notes from doctor and nurse
At 6:45 pm, thirty minutes after the doctor administered the two-milligram dose of Morphine, he called Scott and his wife to tell them, "Grace had a good day." He also informed them he had just given Grace Morphine. Stunned, Scott asked the doctor why Grace was given Morphine and was told, "because she was breathing at 51 breaths a minute." In disbelief, a devastated Scott detailed to attorney Tom Renz the final 42 minutes of Grace's life, explaining:
"Think it through—they caused the breathing to go like this. Of course, I didn't know anything about this combination of drugs at that time. Jessica then called us at 7:20 pm while she was in the room with Grace. She has us on FaceTime. My wife and I are watching and can see Grace, and [we can also see] Jessica panicking because Grace's numbers are tanking. And we're hollering, "get the nurses in the room."
Jessica said, "I've already done that, they won't come in." So we're all hollering at these nurses. She estimated there were about 30 nurses outside the door at that time because of the shift change, and they would not come into the room. We were hollering, "Save our daughter, help her." And they hollered back, "She's DNR [do not resuscitate]." We screamed, "She's not DNR." My wife questioned, "Are you not helping our little girl because she has Down Syndrome?"
This was the first we knew that Grace was DNR. The doctor had put the order in the computer, but we did not sign the DNR. We never asked for a DNR. At approximately 7:22 pm, one of the nurses read the DNR note to Jessica from the computer screen, [implying we couldn't] do anything about it. But the DNR law, which I've looked up, requires them to override a DNR if the patient or a power of attorney requests it. Well, of course we requested it—this is our daughter. They stood outside the room, and it got even worse. They had an armed guard outside the room. So we watched her die on FaceTime."
 Screenshot /Our Amazing Grace / DNR Notes Transcribed from Dr. Shokar's Oct. 13 Hospital Report
Screenshot /Our Amazing Grace / DNR Notes Transcribed from Dr. Shokar's Oct. 13 Hospital Report
To this day, Scott is uncertain of the motivation behind Grace's death. Still, he is convinced the combination of medications set up and caused her death. After all, why did the doctor label Grace DNR, administer Morphine, and then ignore the drug's warnings despite her family's desperate pleading to keep her alive? Why didn't the hospital have the reversal drug Naloxone on hand per Pfizer's instructions? Why was an armed guard posted outside Grace's hospital room door in an apparent effort to prevent staff from helping?
As Scott speculates whether Grace died because of her disability, hospital greed, or rationed care, his investigations have led him to "put together some interesting information that may explain what took place." He explained, "If money was the primary motivator, and there's not a legal method to hold the individuals accountable, the evidence we've put together fits the crime." A page on Grace's website explains Scott's findings further:
"As the U.S. population gets wise to Remdesivir, combined with staffing concerns related to doctors and nurses leaving because of refusing to take the jab and ethical concerns, the medical system will turn to drugs normally used for palliative (end of life) care as the primary tool to accomplish the agenda. This pattern, along with DNR authority taken away from patients/advocates (through government-issued blanket DNR orders on certain population groups), is already happening in the U.K. (see U.K. Attorney, Clare Wills-Harrison explain "end of life drugs and protocols.") Surprisingly, in a Stateline Article dated Mar. 31, 2020, this abuse in the U.S. was already exposed. The article states, "Over the weekend, the U.S. Department of Health and Human Services issued a reminder that people with disabilities have the same worth as everybody else." Why the reminder? "…some U.S. Hospitals already are considering do-not-resuscitate orders for infected patients." Is COVID the convenient excuse to accomplish a portion of the agenda?"
 Screenshot / Our Amazing Grace / Intensivist Conclusion
Screenshot / Our Amazing Grace / Intensivist Conclusion
No Liability & Massive Financial Incentives to COVID Hospitals
Since losing Grace, Scott has done extensive research into the "many abuses, dangers, and financial temptations" occurring in hospitals across the country following the government-funded protocols. As described in Scott's research, according to whistleblowers from the Centers for Medicare and Medicaid Services (CMS), the average CARES Act bonus payment is at least $100,000 per patient. With a combined total of 28,000 beds, St. Elizabeth's hospital is one of 142 hospitals in the Ascension Health System. The national average of hospital beds related to COVID-19 is 18%, and the average COVID-19 hospital stay is 22 days. Remarkably, Ascension health system revenue went up by $1.9 billion from 2020 to 2021, and profit by $4.5 billion. And with money from the U.S. government, its cash flow increased by nearly $9 billion. Scott explained his research into hospital corruption during COVID-19 further, adding:
"Doing the math, Ascension received approximately $8,300,000,000 in each of the two years of COVID! This money is in addition to patient and insurance payments received. This is 'free money' just for following the government's COVID protocol. On a national level, there has been 4,000,000 COVID hospital stays so far (per Dr. Paul Marik—testimony during Ron Johnson's 'Second Opinion' hearing on Jan. 24). Those hospital stays translate to $4,000,000,000,000 [that's 4 Trillion] of our money transferred by the government to their partners facilitating the crime. Where's the motivation to research cures when hospitals and their staff are incentivized to follow an agenda?"
 Screenshot / Our Amazing Grace / The Love of Money? Ascension Health System Exposed
Screenshot / Our Amazing Grace / The Love of Money? Ascension Health System Exposed
 Screenshot / Our Amazing Grace / Medical Liability - summary of immunity from liability
Screenshot / Our Amazing Grace / Medical Liability - summary of immunity from liability
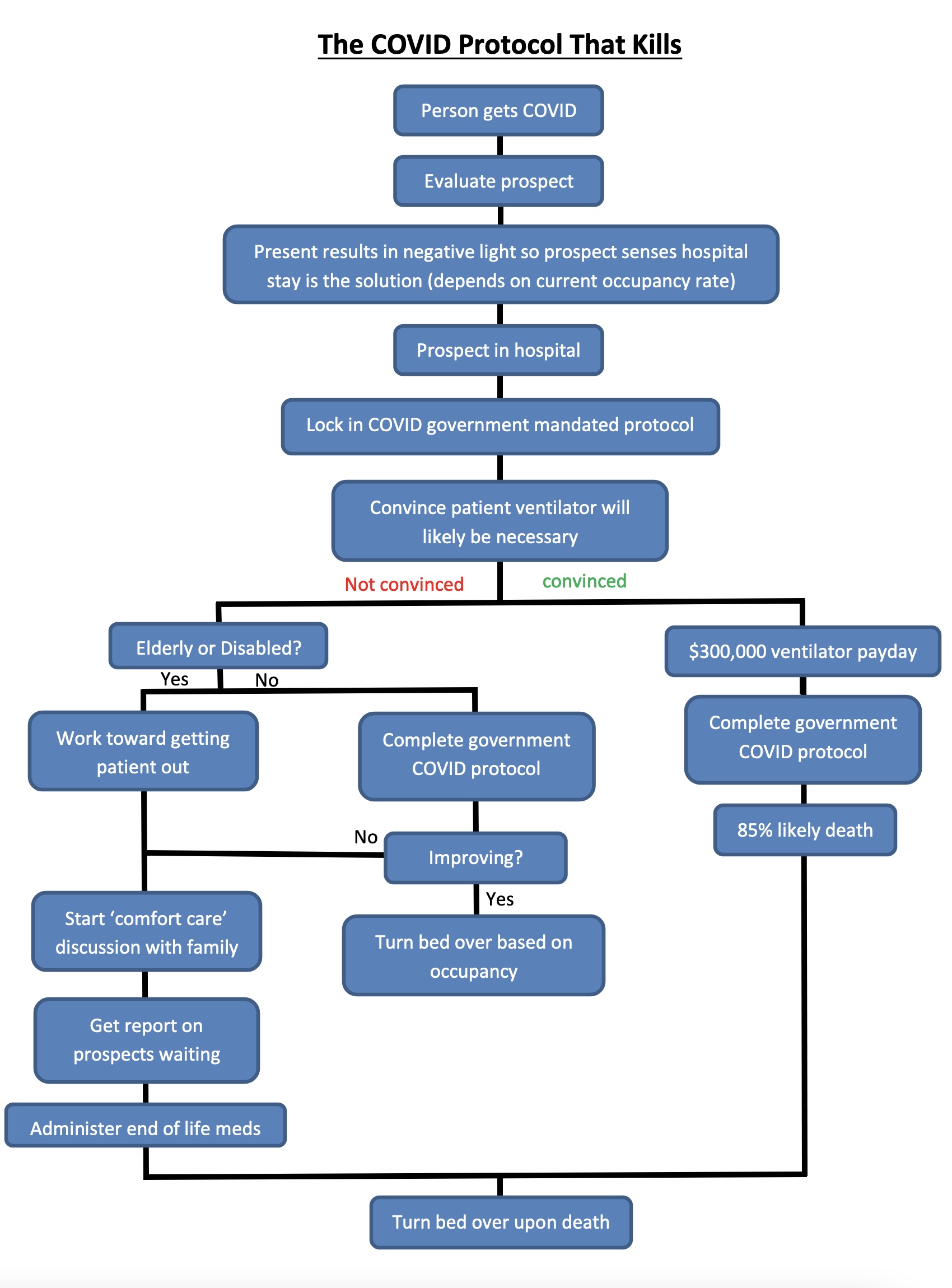
With no accountability, government protocols are based on the WHO's 2005 International Health Regulations, as reported by UncoverDC. In the U.S., WHO statutes direct the Centers for Disease Control (CDC) and the National Institute of Health (NIH) on treatment protocols. From there, hospitals that are federally funded through CMS use coding tied to NIH and CDC-written COVID-19 protocols. If those hospitals take that funding, they must follow those protocols, starting with ICD-10 codes (International Classification of Diseases).
As explained further by attorney Todd Callender in the Epoch Times, these protocols "are passed down hierarchically from the WHO to the CDC and the NIH arising from the Public Readiness and Emergency Preparedness Act (PREP Act) and Health and Human Services authorization to release funding for the declared pandemic that sets the protocols in motion." Callender added:
"The WHO then directs the various state health bodies—in this case, the CDC and NIH—on treatment. This is why every country is responding in the same way at the same time globally; it's a back door to a one-world dictatorial government."
Under the emergency declaration, once these protocols are passed down to the hospitals that accept funding, "patients' rights are waived under the CMS COVID waiver program in conjunction with the PREP and CARES Act, giving participating hospitals legal immunity.
 Our Amazing Grace / Tragedy Money Covid Flowchart
Our Amazing Grace / Tragedy Money Covid Flowchart
The Miracles After Grace's Death
In this tragedy, it is natural to question, "Where was God?" According to Grace's family, "The same place He's always been. He never changes. Grace is with Him today. How do we know? By the fruit she produced. Grace loved Jesus, and that love produced some amazing fruit. Grace's favorite Scripture was 1 John 4:8, which she abbreviated "God is Love."
Steadfast in his faith, Scott is convinced that God has his back and he and his family are "walking accordingly." He said that doors keep opening for him to share what happened to Grace, and so far, he's "documented over 30 miracles that have already taken place." For example, after listening to Sen. Ron Johnson's hearing on Jan. 24, he began looking for a particular intensivist to discuss the deadly combination of medications the hospital gave to Grace. He explained:
"As soon as I was done watching the hearing, I wrote a letter to [the intensivist] and took it out to the mailbox. We live out in the country, and the mail had already been delivered. So I called the post office, and they were already closed. I decided to look the doctor up on a Google search. You can't make this up. I saw a phone number, and I called it. It happened to be his home landline, and his daughter picked up. I asked to speak to her dad, and she said, "who is this?" I replied, "I'm a dad in Wisconsin that lost his daughter in the hospital to a COVID situation." She hollered and asked her dad if he wanted to talk to someone who had lost their daughter. He came to the phone, and we talked. He gave me his email address, and we've had several conversations back and forth since."
Without a doubt, Scott is certain Grace is working through God to shine a light on what happened to her and so many others. Another miracle helping to illuminate the truth occurred after Scott had recently been in the hospital himself for COVID-19. Extremely sick, his experience was entirely different from Grace's because, after what happened to her, he went to a different hospital (St. Vincent's in Green Bay) where his voice mattered. He was given a pill protocol including vitamin E, probiotics, fish oil, and the medicine Baricitinib (for reference, Grace was offered Tocilizumad but Scott rejected it after reviewing studies on the drug. She was never offered Baricitinib). Once recovered, Scott realized he had not received a bill from the hospital—he was expecting it to be approximately $30,000. He called the hospital, and they told him, "they wrote it off to HRSA because we don't have insurance. We used the money for the billboards."
After being informed by a medical malpractice attorney of the slim chances of winning a case on Grace's behalf, the attorney remarked that any money "would be better off spent on billboards" to spread the message about what happened to Grace. With the miracle from St. Vincent's, Scott bought space on the 12 billboards available on Highway 41. The cost is $29,000 for four weeks.

According to their website, the Schara family is in the process of establishing a charitable foundation to honor Grace and share her story, so more people don't die in hospitals during the pandemic. A true light for the Lord while on this earth, Grace's favorite Scripture verse was 1 John 4:8. She would include "God is Love" with many of her works of art. The family's website, called Our Amazing Grace, summarizes their mission, stating:
This is a tragic story. However, we know that God is sovereign and will use this tragedy for good. We envision the foundation we establish in Grace's memory to provide many people with disabilities the opportunity to share their talents and spread the light that Christ has placed in them with the world.


