NYU Langone Health is leading the National Institute of Health's (NIH) investigation of the long-term effects of COVID-19 ("Long COVID"). Dubbed the PASC (Post-Acute Sequelae of SARS-CoV-2 Infection) Initiative, the stated goal of the nearly $450 million project "is to rapidly improve understanding of recovery after SARS-CoV-2 infection and prevent and treat PASC."
Supporting the study, in December 2020, Congress provided $1.15 billion in funding over four years to the NIH to subsidize research into the prolonged health outcomes of SARS-CoV-2 infection. The research will involve adult, pregnant and pediatric patients and include data on clinical information, laboratory tests, and analyses of these patients "in various stages of recovery" after COVID-19 infection. Maintaining that recovery varies significantly from patient to patient, the NIH notes significant post-acute sequelae, documenting:
"Reported symptoms among persons who have been infected with SARS-CoV-2 range from mild to incapacitating, may persist after recovery from acute disease, may involve multiple organs and systems, and can adversely affect overall quality of life. In some cases, new symptoms and findings are reported that appear linked to the timing of acute infection but emerge subsequently and evolve over time."
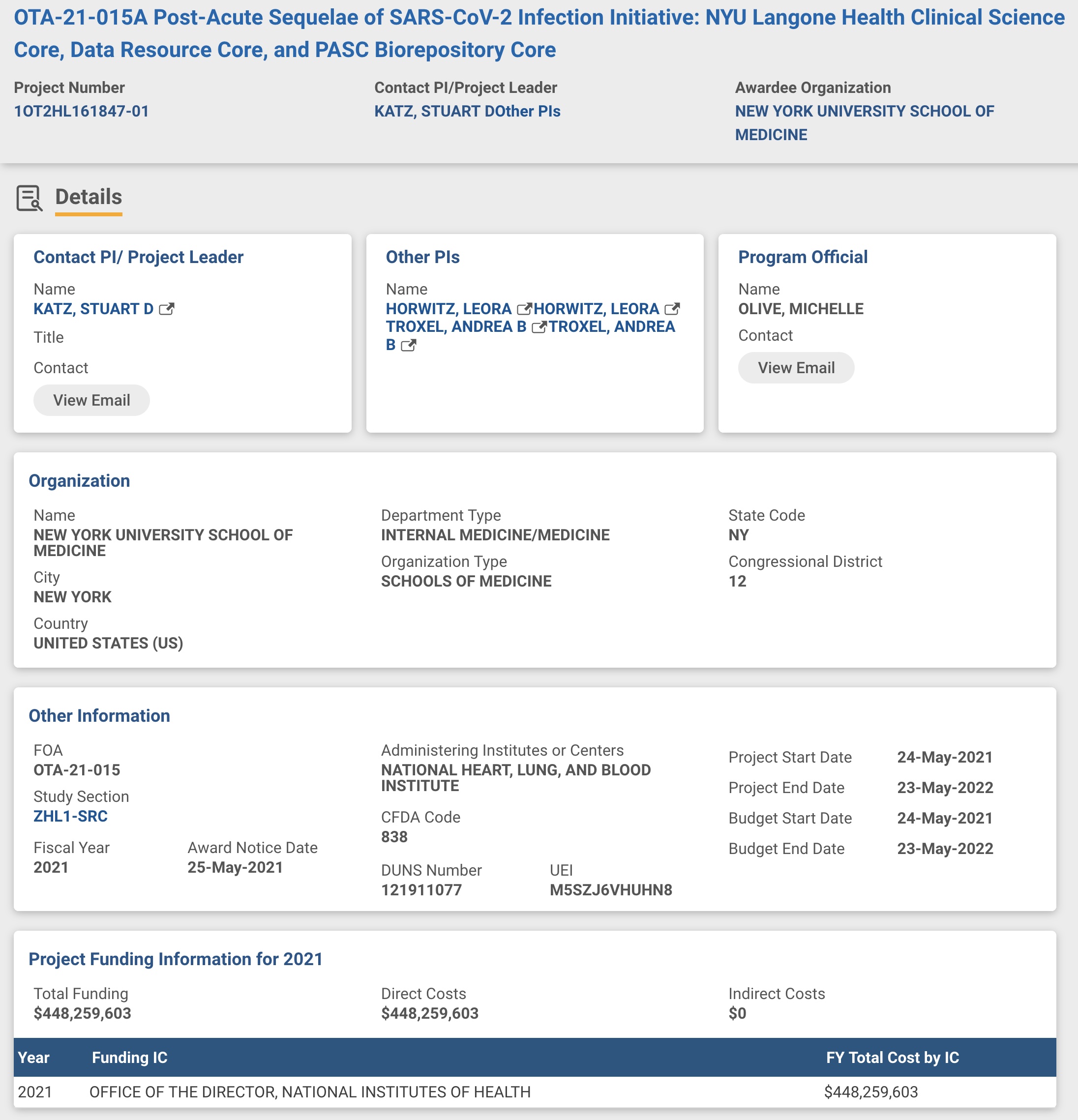 Screenshot / NIH.gov
Screenshot / NIH.gov
 Screenshot / NIAID Post-Acute Sequelae of COVID-19 Workshop, Dec. 3, 2020
Screenshot / NIAID Post-Acute Sequelae of COVID-19 Workshop, Dec. 3, 2020
The NIH study follows a Dec. 3, 2020 virtual workshop hosted by the National Institute of Infectious Diseases (NIAID). Indeed, research and studies into "Long COVID" have been an ongoing focus of NIH Director Francis Collins, who will retire at the end of 2021. In Feb. 2021, when announcing the new NIH initiative to study the emerging symptoms of "Long COVID," Collins remarked:
"We do not know yet the magnitude of the problem, but given the number of individuals of all ages who have been or will be infected with SARS-CoV-2, the coronavirus that causes COVID-19, the public health impact could be profound."
In an effort to summarize what is known about patients who do not fully recover and identify key gaps in NIH knowledge about the effects of COVID-19 after infection, Collins outlined some of the underlying questions the initiative hopes to answer:
- What does the spectrum of recovery from SARS-CoV-2 infection look like across the population?
- How many people continue to have symptoms of COVID-19 or even develop new symptoms after acute SARS-CoV-2 infection?
- What is the underlying biological cause of these prolonged symptoms?
- What makes some people vulnerable to this but not others?
- Does SARS-CoV-2 infection trigger changes in the body that increase the risk of other conditions, such as chronic heart or brain disorders?
 Screenshot / Open VAERS
Screenshot / Open VAERS
Designed to be "fully representative of the diversity of the U.S. population," researchers will study Long COVID symptoms in tens of thousands of patient groups around the country. NYU—serving as the Clinical Science Core (CSC) of the study—explains that symptoms like "fatigue, shortness of breath, "brain fog," sleep disorders, fevers, gastrointestinal symptoms, anxiety, and depression" can persist for months after recovery from the initial COVID-19 illness. As of Dec. 28, 2021, roughly 53 million Americans have tested positive for COVID-19, with nearly 800,000 deaths.
In agreement with the NIH that "Long COVID" is around to stay, the Biden administration announced in July that "Long COVID" patients living in the U.S. are entitled to disability rights and resources under federal law, including the Americans with Disabilities Act (ADA). Pleased with Biden's decision, two groups focused on COVID-19 chronic illness, Body Politic and Patient Led Research Collaborative, describe "Long COVID" as "one of the largest mass disabling events in modern history."
A newly formed central part of the NIH study is its RECOVER initiative (which stands for Researching COVID to Enhance Recovery). A central feature of RECOVER is the creation of the SARS-CoV-2 Recovery Cohort. Despite studies suggesting Long COVID is less common in children and adolescents, another critical aspect of RECOVER is the development of the "pediatric main protocol for study of Long COVID in children."
Meanwhile, as fully vaccinated individuals are reinfected with COVID-19, reports suggest they are also not safe from developing "Long COVID." With the design of the main study protocols complete, Stuart D. Katz, MD—director of NYU Langone's heart failure program and principal investigator for the RECOVER CSC—underscored the urgent need of the PASC study, stating:
"The goal of the newly funded RECOVER studies, in adults, children, and in pregnant women, is to fully understand the long-term consequences of COVID-19 and the pace and extent of recovery over time. We recognize the need to urgently begin nationwide enrollment for collection of the information needed to better understand and improve treatment for long COVID-19."


